Appendicitis in Pregnancy: Early Signs, Causes & When to Seek Emergency Care
Overview
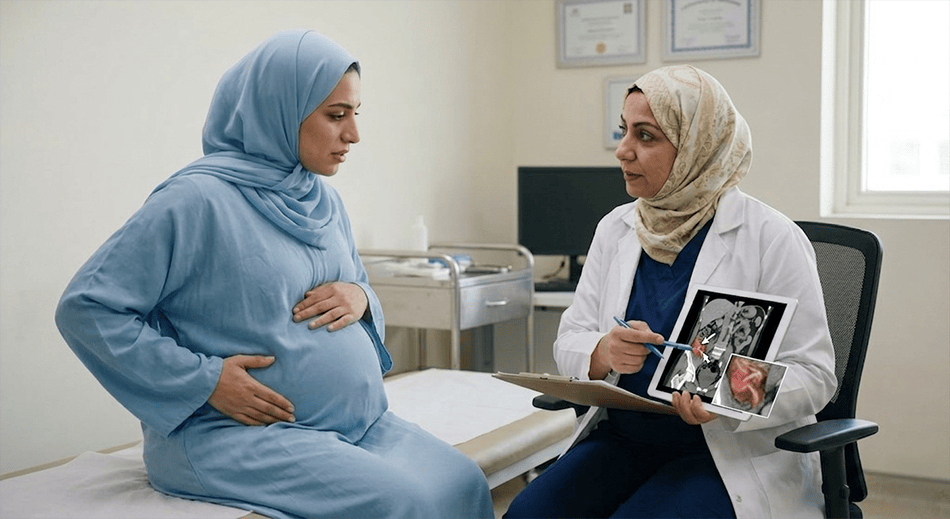
Appendicitis is a medical emergency that requires prompt evaluation and treatment. It is the most common non-obstetric surgical emergency during pregnancy. Failure to promptly treat appendicitis places both the mother and fetus at significant risk. Early recognition of symptoms and an awareness of how pregnancy can alter the presentation of appendicitis may allow pregnant women to receive appropriate care in a timely manner.
What Is Appendicitis?
The appendix is a small, finger-shaped pouch connected to the cecum (the beginning part of the colon) on the lower right side of the abdominal wall. Appendicitis develops when the appendix becomes inflamed. Typically, this inflammation results from some form of blockage inside the appendix. When the appendix becomes inflamed, it may become swollen. Bacteria may accumulate inside the appendix. If left untreated, appendicitis may lead to rupture of the appendix. Rupture of the appendix is a serious medical emergency. Upon rupture of the appendix, bacteria enter the abdominal cavity. The presence of bacteria in the abdominal cavity causes severe infection known as peritonitis. Peritonitis complicates pregnancy. There is an increased risk of miscarriage or pre-term delivery when there is severe infection, such as peritonitis due to a ruptured appendix, during pregnancy.
Causes of Appendicitis in Pregnancy
Appendicitis during pregnancy can arise from similar factors as in the general population. These causes are primarily related to some form of blockage in the lumen of the appendix that leads to subsequent inflammation. Many different types of blockages can occur. Some examples include hardened feces or mucus buildup, enlarged lymph nodes following an infectious process, and parasites. Pregnancy does not directly cause appendicitis. However, as the uterus expands, it may move the appendix upward toward the liver and to the right side of the body. This positioning of the appendix can make diagnosing appendicitis difficult because pain from appendicitis may not appear in its typical anatomical region.
Early Signs of Appendicitis in Pregnancy
Prompt and proper diagnosis of appendicitis in pregnant women is important to reduce the risk of complications for both the mother and her unborn child.
The common Signs of appendicitis include:
- Right lower quadrant abdominal pain (Pain begins near the navel and radiates to the lower right abdomen)
- Nausea and vomiting
- Diminished interest in food
- Low-grade Fever
- Sensitivity overlying the appendix when palpated
Because many pregnant women experience nausea, bloating, and round ligament pains that mimic symptoms of appendicitis, prompt evaluation and diagnosis are crucial. If abdominal pain persists, worsens, or is severe in nature, do not wait to see if your discomfort resolves. Seek emergency medical assistance immediately.
How Appendicitis Symptoms Differ During Pregnancy
As mentioned previously, pregnancy alters both where and how appendicitis pain manifests. Due to the increasing size of the uterus during pregnancy, the appendix may be displaced upward and to the right of its usual anatomical location. Therefore, by the third trimester, appendicitis pain may manifest in either the middle or upper right aspects of the abdomen. Other differences in symptoms during pregnancy include:
- A decrease in localized abdominal tenderness secondary to the separation between the appendix and the abdominal wall produced by the expanding uterus
- Difficulty in distinguishing nausea and vomiting caused by appendicitis from those caused by morning sickness
- A fever may be milder in the early stages of appendicitis during pregnancy
- Decreased muscle guarding and abdominal wall rigidity compared to nonpregnant individuals with appendicitis
Because these changes can make diagnosis more challenging, early evaluation is essential, and clinicians should consider appendicitis as a possible cause of persistent or worsening abdominal pain in pregnancy, particularly during late gestation.
Diagnosing Appendicitis in Pregnant Women
Appendicitis during pregnancy is often more difficult to evaluate than in non-pregnant patients. Diagnoses are made using clinical evaluations combined with laboratory testing and/or imaging studies.
White blood cell counts (WBC) increase in response to infection or inflammation. WBC counts also increase normally during pregnancy. Hence, abnormal WBC counts cannot confirm a diagnosis of appendicitis alone.
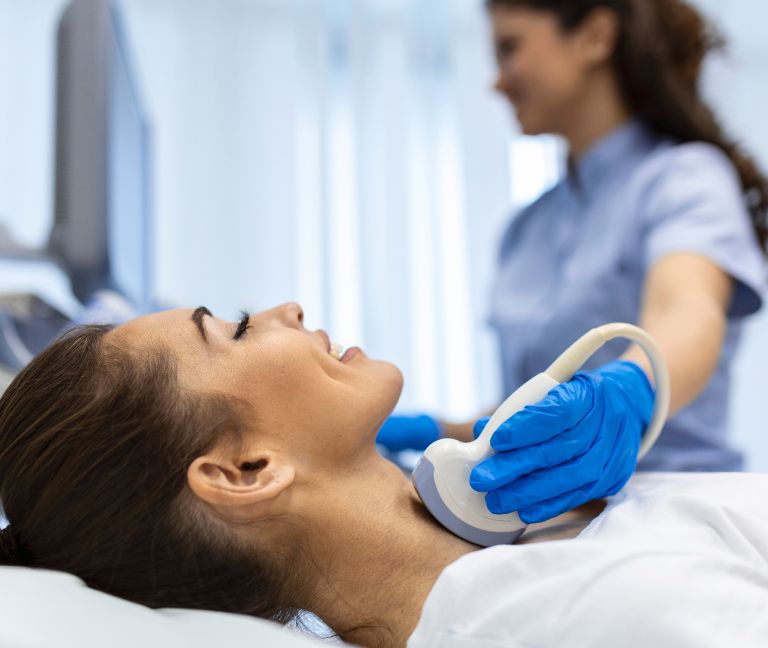
Ultrasound is utilized as the initial imaging study in pregnant patients suspected of having appendicitis since it is free from ionizing radiation. Ultrasound is successful in detecting appendicitis through early gestational age; however, as the uterus enlarges with advancing gestational age, visualization of the appendix decreases, thereby limiting the utility of ultrasound in advanced gestations.
When Ultrasound findings suggest possible appendicitis, magnetic resonance imaging (MRI) is employed as a secondary imaging modality. MRI can provide detailed images without subjecting the fetus to ionizing radiation. CT may be considered when MRI is unavailable or an urgent diagnosis is needed, with fetal radiation exposure minimized as much as possible. Both delayed diagnosis and failure to initiate prompt treatment greatly increase the risk of rupture of the appendix and resultant maternal-fetal complications.
Treatment Options for Appendicitis in Pregnancy
Surgical removal of the inflamed appendix via appendectomy is the established treatment for appendicitis in pregnant patients. General surgeons work in conjunction with obstetricians to safely perform an appendectomy, utilizing either an open surgical technique or a minimally invasive laparoscopic technique based upon patient-specific criteria.
The choice between open and laparoscopic appendectomy depends upon several variables, including gestational age at the time of surgery and whether perforation occurred prior to surgery.
Studies have demonstrated that certain patients with uncomplicated appendicitis may be successfully treated with antibiotic therapy alone. However, given the relatively high recurrence rates and risk of rupture seen with conservative treatment options during pregnancy, routine antibiotic therapy without surgical intervention is not commonly recommended. Surgical intervention remains the gold-standard method for managing acute appendicitis during pregnancy.
Recovery After Appendicitis Surgery During Pregnancy
Recovery from an appendectomy during Pregnancy varies according to gestational age at the time of surgery, type of surgical technique performed (laparoscopic vs open), and whether rupture occurred prior to surgery. Patients undergoing laparoscopic procedures typically spend 1-2 days hospitalized postoperatively. Hospitalizations lasting longer than 2 days are often required for those requiring open surgery or when a rupture occurred prior to surgery. Pain control regimens must be cautiously chosen to avoid adverse effects on fetal development. Obstetrical monitoring includes fetal heart rate assessments and uterine contractions throughout the post-operative period.
Physiologic limitations exist regarding physical activity post-surgically. Avoidance of strenuous physical exertion and lifting heavy objects is recommended until sufficient healing has taken place at the surgical site. Return to regular daily activities is usually feasible for most patients within 7-14 days following discharge, depending on the individual's progress of recovery.
Recovery time after an appendectomy is prolonged for women whose appendix ruptured prior to surgery. In addition to prolonged recovery time, women who undergo surgery after their appendix ruptures often require IV antibiotics for extended periods to resolve resulting intra-abdominal infections.
How Common Is Appendicitis During Pregnancy?
Approximately 1 in every 500-1000 pregnancies develops appendicitis. Although uncommon, appendicitis is the most prevalent reason for nonobstetric abdominal surgeries during Pregnancy.